
Tooth Sensitivity to Cold Air: Is It Serious?
Cold sensitivity in teeth is most often caused by exposed dentin, enamel wear, or gum recession, but when it becomes localized, persistent, or painful, it may signal decay, cracks, or nerve involvement. The key is early identification and targeted treatment, which can prevent more serious dental complications.
Key Takeaways
- Tooth sensitivity to cold most often results from exposed dentin or irritated nerve tissue, not simply "weak enamel."
- Enamel erosion, gum recession, and microscopic cracks are among the most frequent underlying causes.
- Sinus infections can cause referred pain to the upper teeth, often mimicking dental issues.
- Sudden sensitivity should always be evaluated, as it may indicate structural or bacterial damage.
- Proper diagnosis depends on distinguishing between sinus-related pressure and true dental pain.
Why are my teeth sensitive to cold, and what does it mean?
You take a sip of cold water, and suddenly, a sharp, almost electric sensation shoots through your tooth. It disappears quickly, but it leaves a question behind: what exactly just happened? Tooth sensitivity to cold is not random. It is a signal. And in dentistry, signals matter.
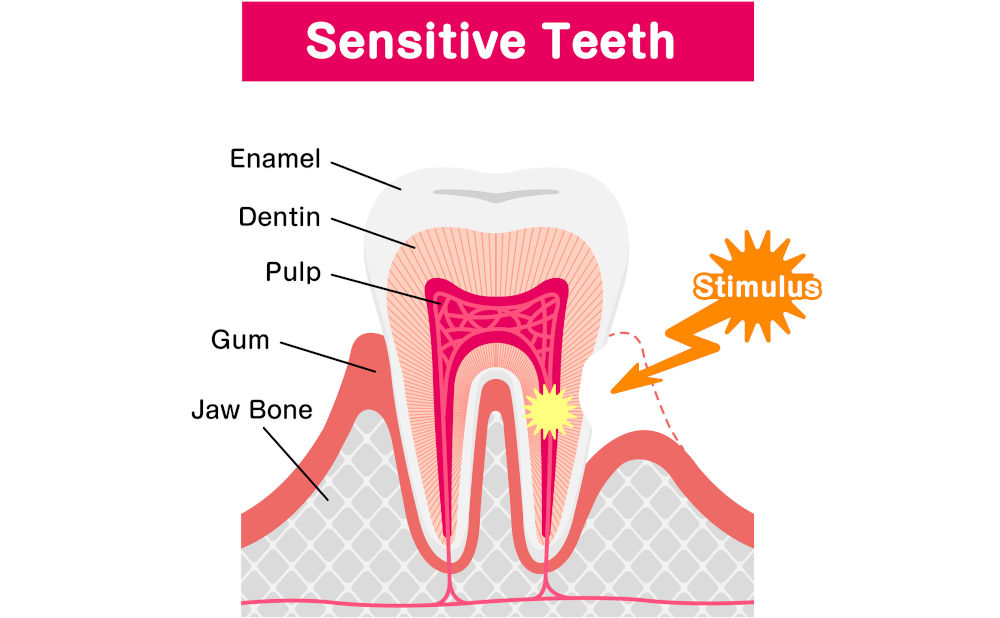
To understand this, we need to look beyond the surface. Teeth are not solid blocks; they are layered, living structures. The outermost layer, enamel, is the hardest substance in the human body. Beneath it lies dentin, a porous tissue filled with microscopic tubules that connect directly to the nerve inside the pulp. When enamel is compromised or gums recede, these tubules become exposed. Cold stimuli travel through them rapidly, triggering the nerve.
Now, an important point this process is not necessarily a sign of advanced disease. In many cases, it reflects early-stage structural changes that are still manageable. However, ignoring it allows the underlying issue to progress.
What happens inside the tooth?
Inside every tooth is a complex biological system. The pulp contains nerves and blood vessels that respond to temperature changes. According to research published in the Journal of Clinical Periodontology, fluid movement within dentinal tubules, known as the hydrodynamic mechanism, is the primary cause of sensitivity. When cold air or liquid contacts exposed dentin, it causes rapid fluid shifts, which stimulate nerve endings.
But why does dentin become exposed in the first place? There are several pathways:
- Gradual enamel erosion due to acidic foods or beverages
- Mechanical wear from aggressive brushing
- Gum recession exposing the root surface
- Early-stage decay weakens protective layers
Each of these creates a pathway for stimuli to reach the nerve. And interestingly, sensitivity can fluctuate; some days it feels intense, other days barely noticeable. This variability often reflects changes in inflammation levels or external triggers.
From a clinical perspective, sensitivity is not just about discomfort; it’s a diagnostic clue. Dentists use it to identify early enamel breakdown, occlusal stress, or gingival changes before they become severe.
As noted by Dr. Amir Guorgui, BSC, DMD, MACSD, from Pickering Smile Centre: “Tooth sensitivity is often the first indication that the protective layers of the tooth have been compromised. Addressing it early allows us to prevent more complex issues from developing.”
And that’s the key takeaway here: sensitivity is not the problem itself. It’s the message your body is sending.
Why do my teeth hurt when I have a cold or sinus infection?
This is where things get confusing. You have a cold, maybe sinus pressure, and suddenly your upper teeth start to ache. Naturally, it feels like a dental issue. But in many cases, the teeth themselves are not the source of the problem.
The roots of the upper molars sit very close to the maxillary sinuses. In some individuals, they are separated by only a thin layer of bone or sometimes just soft tissue. When the sinuses become inflamed due to infection or congestion, pressure builds. That pressure presses downward, affecting the nerves that also serve the teeth.
The result? Pain that feels like it’s coming directly from your teeth.
Sinus vs tooth pain differences
So how do you tell the difference? This is where clinical evaluation and a bit of self-awareness come into play.
Sinus-related pain tends to:
- Affect multiple upper teeth at once
- Intensify when bending forward or lying down
- Be accompanied by nasal congestion or facial pressure
- Feel dull, throbbing, or pressure-like rather than sharp
In contrast, true dental pain is usually:
- Localized to one specific tooth
- Triggered by temperature or biting
- Sharp or persistent
- Independent of sinus symptoms
Dr. James C.H. Ko DDS explains: “Patients often assume tooth pain during a cold is due to decay, but in many cases, it is referred pain from sinus inflammation. A proper examination helps distinguish between the two and prevents unnecessary treatment.”
Now, here’s something worth noting: sometimes, both conditions can coexist. A tooth with mild sensitivity may feel significantly worse during a sinus infection due to increased pressure. This overlap makes professional diagnosis even more important.
What are the most common causes of sudden tooth sensitivity to cold?
Sudden sensitivity can feel alarming. One day everything seems fine, and the next, cold drinks become uncomfortable. But in most cases, this change is not as sudden as it seems; it’s the result of gradual processes reaching a tipping point.
Let’s break down the most common causes.
Primary causes of sensitivity
| Cause | What Happens | Key Indicator |
|---|---|---|
| Enamel erosion | Acid wears down protective enamel | Sensitivity to cold and sweets |
| Cavities | Bacterial decay penetrates enamel | Localized pain, possible discoloration |
| Gum recession | The root surface becomes exposed | Sensitivity near the gumline |
| Cracked tooth | Structural damage exposes dentin | Pain when biting or releasing pressure |
Each of these affects the tooth’s protective barrier. Once that barrier is compromised, external stimuli can reach the nerve more easily.
Research published in the Journal of Dentistry indicates that dentin hypersensitivity affects up to 57% of adults at some point, with higher prevalence in individuals with gum recession or dietary acid exposure.
Most overlooked causes
Some causes are less obvious and often missed during early stages.
- Teeth grinding (bruxism), which creates microfractures
- Whitening products used excessively or incorrectly
- Recent dental procedures, such as cleanings or restorations
- Orthodontic movement is causing temporary sensitivity
And here’s an interesting nuance: lifestyle plays a significant role. Frequent consumption of acidic beverages, such as carbonated drinks and citrus juices, gradually softens enamel. Combine that with brushing immediately afterward, and enamel wear accelerates.
Another overlooked factor is brushing technique. Many people assume that brushing harder cleans better. In reality, it can lead to enamel abrasion and gum recession over time.
From a clinical standpoint, identifying the cause requires a comprehensive assessment. Sensitivity is rarely caused by a single factor; it is usually a combination of mechanical, chemical, and biological influences.
What’s the result of ignoring it? The condition may progress from reversible sensitivity to irreversible pulp damage, requiring more complex treatment.
And that brings us back to the central idea: early recognition changes outcomes. Sensitivity is not just discomfort; it is an opportunity for prevention.
Can a single tooth being sensitive to cold indicate a serious problem?
It’s easy to dismiss sensitivity when it affects several teeth; many people assume it’s related to enamel wear or diet. But when one specific tooth reacts sharply to cold, the situation becomes more precise and often more concerning.
Localized sensitivity typically indicates a structural or pathological issue affecting that specific tooth. Unlike generalized sensitivity, which may stem from widespread enamel thinning, single-tooth discomfort often suggests something more focused: decay, a crack, or even early infection.
One of the most common causes is dental caries. When decay penetrates the enamel and reaches dentin, the protective barrier is compromised. Cold stimuli can then reach the nerve more easily, resulting in a quick, sharp pain. Another frequent cause is a cracked tooth, sometimes so small it is not visible without magnification. These microfractures allow temperature changes to travel deeper into the tooth.
And then there’s the possibility of pulp inflammation. When bacteria or trauma irritate the pulp, the nerve becomes hypersensitive. At this stage, sensitivity may still be reversible but only if addressed promptly.
Warning signs
Not all sensitivity signals the same level of urgency. However, certain symptoms should not be ignored:
- Pain that lingers after exposure to cold
- Sensitivity that worsens over time instead of improving
- Discomfort when biting or releasing pressure
- Visible dark spots or structural changes in the tooth
- Swelling or tenderness in the surrounding gum tissue
According to findings published in the International Endodontic Journal, prolonged sensitivity to thermal stimuli is often associated with pulpal inflammation and may indicate progression toward irreversible pulpitis.
Dr. Amir Guorgui notes: “When sensitivity is isolated to one tooth, we look more closely for structural damage or decay. Early detection allows us to intervene before the nerve becomes permanently affected.”
What’s often overlooked is how quickly things can escalate. A small cavity or crack can remain asymptomatic for months and then suddenly become sensitive when it reaches dentin. That “sudden” change is actually the result of a long, silent process.
What dental conditions make teeth very sensitive to cold?
Some conditions don’t just cause mild discomfort; they make cold exposure genuinely unpleasant. Understanding these conditions helps explain why sensitivity can vary so dramatically from one patient to another.
Condition breakdown
| Condition | Mechanism | Severity Level | Typical Symptoms |
|---|---|---|---|
| Cavities | Bacterial breakdown of enamel and dentin | Moderate to high | Localized sensitivity, pain with sweets |
| Exposed roots | Gum recession reveals dentin | Moderate | Sensitivity near gumline, especially to cold air |
| Worn fillings | Breakdown of restoration margins | Moderate | Sensitivity around treated teeth |
| Cracked teeth | Structural fractures expose inner layers | High | Sharp pain when biting, temperature sensitivity |
| Enamel erosion | Chemical wear from acids | Mild to moderate | Generalized sensitivity, smooth enamel surfaces |
Each condition affects the tooth differently, but the underlying principle remains the same: loss of protection leads to nerve stimulation.
An interesting clinical observation: patients with multiple contributing factors often experience heightened sensitivity. For example, someone with mild gum recession and enamel erosion may report severe discomfort, even if each condition alone seems minor.
How can you prevent your teeth from becoming sensitive to cold?
Prevention is where dentistry becomes truly proactive. And the good news? Most causes of sensitivity are manageable with consistent habits and early care.
It starts with understanding that enamel does not regenerate. Once it is worn away, it cannot grow back. That means prevention is not just helpful, it is essential.
From a clinical standpoint, three areas matter most: hygiene, diet, and regular dental monitoring.
Daily routine checklist
A practical approach makes all the difference. Here’s what an effective daily routine looks like:
- Brush twice daily using a soft-bristle toothbrush
- Use fluoride toothpaste to strengthen enamel
- Avoid brushing immediately after acidic meals or drinks
- Floss daily to reduce plaque and gum inflammation
- Limit acidic beverages such as soda and citrus juices
- Stay hydrated to support saliva production
- Use desensitizing toothpaste if sensitivity is present
Diet also plays a surprisingly large role. Frequent snacking, especially on acidic or sugary foods, creates a constant cycle of enamel demineralization. Giving your teeth time to recover between meals helps maintain their protective structure.
Regular dental visits complete the picture. Professional cleanings remove plaque buildup that contributes to gum recession, while early examinations detect minor issues before they become symptomatic.
And here’s the honest conclusion: most sensitivity cases are preventable. But prevention requires consistency. Small daily habits, repeated over time, determine whether enamel remains intact or gradually wears away.
When should you see a dentist for tooth sensitivity?
There’s a moment many patients recognize you feel sensitivity, you pause, and then you wonder: is this something that will pass, or something that needs attention? The difficulty lies in the fact that tooth sensitivity exists on a spectrum. In some cases, it is mild and temporary. In others, it is the first visible sign of a developing dental condition.
Timing matters more than most people expect. Sensitivity that appears briefly after whitening, a cleaning, or dietary changes may resolve on its own. However, persistent or worsening symptoms suggest an underlying issue that requires clinical evaluation. The challenge is distinguishing between these scenarios early enough to prevent escalation.
From a diagnostic perspective, dentists look for patterns, frequency, duration, and triggers. Sensitivity that occurs only occasionally and disappears quickly is often less concerning. But when discomfort becomes predictable or persists after exposure to cold, it signals deeper involvement of the dentin or pulp.
What to expect at the appointment
A dental appointment for sensitivity is not just about identifying pain—it’s about identifying the cause. The process typically involves several steps:
- Clinical examination of enamel, gums, and restorations
- Thermal testing to assess nerve response
- Bite evaluation to detect cracks or occlusal stress
- X-rays to identify decay or internal damage
There are also clear indicators that require more urgent care:
- Pain that lingers for more than 30 seconds after cold exposure
- Spontaneous pain without any trigger
- Swelling, fever, or signs of infection
- Sensitivity combined with visible damage or trauma
Dr. Amir Guorgui explains: “The key is not to wait for pain to become severe. Sensitivity is often the earliest stage where intervention is simplest and most effective.”
And that’s the practical takeaway early visits are not about overreacting. They are about preventing complexity.

How does professional dental care in Pickering help treat sensitivity?
Treatment is not one-size-fits-all. In fact, one of the most important aspects of managing sensitivity is tailoring the approach to the specific cause. This is where professional dental care becomes essential, particularly in a setting that combines clinical experience with modern diagnostic tools.
At Pickering Smile Centre, treatment begins with a comprehensive assessment rather than immediate intervention. Understanding whether sensitivity is caused by enamel erosion, gum recession, or structural damage determines the course of care.
Treatment process overview
The treatment pathway typically follows a structured approach:
- Diagnosis – Identifying the exact cause through examination and imaging
- Immediate relief – Application of desensitizing agents or fluoride varnishes
- Structural treatment – Addressing cavities, cracks, or failing restorations
- Preventive strategy – Adjusting hygiene practices and dietary habits
Common in-office treatments may include:
- Fluoride applications to strengthen enamel
- Dental bonding to cover exposed dentin
- Replacement of worn fillings
- Night guards for patients with bruxism
Another important aspect is patient education. Technology enables more precise diagnostics, but long-term success depends on how well patients understand and adhere to preventive strategies.
And this is where local care makes a difference. Ongoing monitoring ensures that small changes are detected early, reducing the likelihood of invasive procedures later.
What is the best way to manage long-term tooth sensitivity?
Long-term management is not about eliminating sensitivity overnight. It’s about controlling the factors that cause it and maintaining that control consistently.
One of the most important concepts in dentistry is that tooth structure changes over time. Enamel wears, gums shift, and restorations age. Managing sensitivity means adapting to these changes rather than reacting to them after symptoms appear.
Lifestyle + dental combo
Sustainable management comes from combining daily habits with professional care:
- Maintain consistent oral hygiene with gentle brushing techniques
- Use fluoride or potassium nitrate toothpaste regularly
- Limit acidic food and beverage exposure
- Schedule routine dental check-ups and cleanings
- Address grinding or clenching with protective appliances
What’s often underestimated is the role of consistency. A single change, like switching toothpaste, may help temporarily. But lasting improvement requires multiple aligned habits over time.
There is also a behavioural component. Patients who modify brushing pressure, adjust their diet, and follow professional recommendations tend to experience significantly better outcomes.
And here’s an important nuance—sensitivity may not disappear completely in all cases. However, it can almost always be reduced to a level where it no longer interferes with daily life.
What should you do if your teeth are sensitive to cold?
Cold sensitivity is not just an inconvenience it is a clinical signal. It reflects changes in tooth structure, gum position, or nerve response. And while it may start as a mild, occasional discomfort, it can progress if left unaddressed.
The causes vary, including enamel erosion, gum recession, decay, cracks, or even sinus-related pressure. Each requires a different approach, which is why accurate diagnosis is essential. Treatment may range from simple preventive care to restorative procedures, depending on the severity and origin of the issue.
Prevention, however, remains the most effective strategy. Consistent oral hygiene, mindful dietary choices, and regular dental visits form the foundation of long-term dental health. When these elements are in place, the risk of sensitivity and its progression decreases significantly.
If sensitivity appears suddenly, becomes localized, or worsens, seeking professional evaluation is the most reliable next step. Early intervention not only resolves discomfort but also prevents more complex conditions from developing.
References
- Canadian Dental Association – https://www.cda-adc.ca
- Journal of Dentistry – https://www.journals.elsevier.com/journal-of-dentistry
- Journal of Clinical Periodontology – https://onlinelibrary.wiley.com
- Journal of Endodontics – https://www.jendodon.com
- Journal of the American Dental Association (JADA) – https://jada.ada.org
FAQ
1. Is tooth sensitivity to cold always a sign of a cavity?
Not always. While cavities can cause sensitivity, other factors like enamel erosion or gum recession are also common causes.
2. Why does only one tooth hurt when I drink something cold?
Localized sensitivity often indicates a specific issue, such as a crack, cavity, or worn filling, affecting that tooth.
3. Can sinus infections really cause tooth pain?
Yes, especially in the upper teeth. Sinus pressure can affect shared nerve pathways, creating referred pain.
4. Does sensitive toothpaste actually work?
Yes, especially those containing potassium nitrate or fluoride, which help reduce nerve response over time.
5. When should I see a dentist for sensitivity?
If sensitivity is persistent, worsening, or localized, it is best to schedule an examination promptly.
